February 2024
Three Grades of Ankle Sprains
An ankle sprain occurs when one or more ankle ligament gets overly stretched. Ligaments are strong bands of tissue that bind and support the bones and other structures that make up the ankle. In more severe ankle sprains, the ligament(s) tear—either partially or completely—and there may be an audible popping noise at the moment of injury.
Ankle sprains are quite common and can occur when the ankle rolls outwardly (eversion) or inwardly (inversion), causing the ligament(s) to stretch beyond normal limits, or even tear. Falls, twists, or blows to the ankle during sports or other activities can cause this injury, as well as wearing improper footwear, running on uneven surfaces, or having weak ankles.
Depending on the injury’s severity, an ankle sprain will be classified as Grade I, Grade II, or Grade III. Grade I sprains involve ligament(s) being overly stretched but not torn, with symptoms of mild pain, swelling, and ankle instability. There may also be some difficulty bearing weight. A Grade II sprain usually involves a partial tear of the ligament which brings more intensity in these symptoms, along with possible bruising. With a Grade III sprain, the ligament is completely torn, the symptoms are severe, and it may not be possible to put weight on the affected foot at all.
To diagnose and grade an ankle sprain, a podiatrist will perform a physical examination, checking for tenderness and range of motion in the ankle. For more severe sprains, X-rays or other imaging studies may be necessary.
It is vitally important to have an ankle sprain treated properly as improper healing often leads to future ankle sprains and possibly even chronic ankle stability. Treatment for an ankle sprain will vary, depending on its severity, and may include the RICE method (Rest/Ice/Compression/Elevation), physical therapy, bracing, medications, and possibly even surgery to repair a torn ligament. Rehabilitation is very important for the sprain to heal properly and to restore functionality.
Managing Various Grades of Ankle Sprains
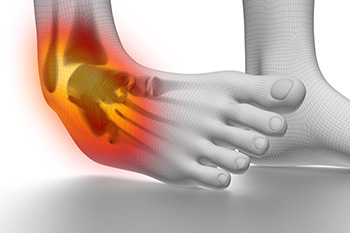
Ankle sprains are common injuries that can disrupt daily activities and sports participation. Effective management of ankle sprains involves understanding the severity of the injury and implementing appropriate treatment strategies. Ankle sprains are often classified into three grades, based on the extent of ligament damage. Grade I sprains involve mild stretching or microscopic tears of the ligaments, resulting in minimal swelling and pain. Grade II sprains involve partial tearing of the ligaments, leading to moderate swelling, pain, and instability. Grade III sprains are the most severe, involving complete tearing of the ligaments, significant swelling, and joint instability. Management of ankle sprains typically begins with elevation which may help to reduce any existing swelling. In severe cases, immobilization with a brace or boot may be necessary to facilitate healing. Gradual return to weight-bearing activities and sports should be guided by pain tolerance and functional improvement, aiming to prevent recurrent injuries and promote long-term ankle health. If you have sprained an ankle, it is suggested that you consult a podiatrist who can determine the grade of the sprain and offer appropriate treatment methods.
Although ankle sprains are common, they aren’t always minor injuries. If you need your ankle injury looked at, contact Dr. Ronald K. Olm from Grand Traverse Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains are the result of a tear in the ligaments within the ankle. These injuries may happen when you make a rapid shifting movement while your foot is planted. A less common way to sprain your ankle is when your ankle rolls inward while your foot turns outward.
What Are the Symptoms?
- Pain at the sight of the tear
- Bruising/Swelling
- Ankle area is tender to touch
- In severe cases, may hear/feel something tear
- Skin discoloration
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
In many cases, the RICE method (Rest, Ice, Compression, and Elevate) is used to treat ankle sprains. However, you should see a podiatrist to see which treatment option would work best with your injury. In severe cases, surgery may be required.
It is important to ask your doctor about rehab options after you receive treatment for your injury. Stretching, strength training, and balance exercises may help the ankle heal while also preventing further injury.
If you have any questions, please feel free to contact one of our offices located in Traverse City and Kalkaska, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Past, Present, and Future of Diabetic Foot Ulcer Treatment

The surge in global diabetes has led to a rise in diabetic foot ulcers, posing significant health challenges. In the mid-19th century, Marchal de Calvi and Thomas Hodgkin identified the link between diabetes and foot gangrene, paving the way for pioneering treatments like Frederick Treves' sharp debridement method. Treves emphasized pressure relief and patient education. The discovery of insulin in the 20th century improved diabetic patients' lives but also increased foot disease cases. Elliot Joslin established the first foot clinic in 1928, advocating a multidisciplinary approach. Penicillin's discovery in 1928 revolutionized infection treatment, reducing amputation rates. Revascularization techniques and limb salvage became critical, with Frank Wheelock pioneering bypass grafts. Topical negative pressure therapy emerged in the 1990s, aiding wound healing. Despite advancements, chronic diabetic ulcers remain a challenge, with ongoing research for new treatments. Current treatment involves a multidisciplinary approach, controlling diabetes, and utilizing various wound care methods. Challenges persist, underscoring the importance of diabetics scheduling routine appointments with a podiatrist for foot examinations and specialized care.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Ronald K. Olm from Grand Traverse Foot & Ankle Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in Traverse City and Kalkaska, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Solutions for Cracked Heels
Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
Is There a Link Between Vitamin B-3 Deficiency and Cracked Heels?
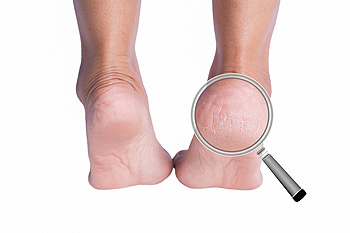
Vitamin B-3, also known as niacin, plays a vital role in maintaining healthy skin and overall well-being. A deficiency in this essential nutrient can lead to various skin issues, including cracked heels. Cracked heels, characterized by dry, fissured skin around the edges of the heel, often result from inadequate moisture retention and weakened skin integrity. Vitamin B-3 deficiency exacerbates this condition by impairing the skin's ability to retain moisture and regenerate cells effectively. Incorporating niacin-rich foods such as meat, fish, nuts, and fortified cereals into the diet can help prevent vitamin B-3 deficiency and alleviate cracked heels. Understanding the connection between vitamin B-3 deficiency and cracked heels underscores the importance of maintaining a balanced diet and proper skin care regimen for optimal foot health. If you have developed cracked heels, it is suggested that you consult a podiatrist for successful treatment methods, in addition to determining if there is an adequate amount of vitamin B-3 in your daily food intake, and how it may relate to cracked heels.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Dr. Ronald K. Olm from Grand Traverse Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact one of our offices located in Traverse City and Kalkaska, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Treat Your Toenail Fungus
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
Types of Toenail Fungus
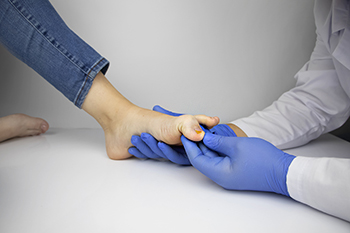
Toenail fungus, medically termed onychomycosis or tinea unguium, is a common fungal infection that affects approximately 14 percent of people, as reported by the Centers for Disease Control and Prevention. While typically not a serious health concern, toenail fungus can cause cosmetic issues as well as discomfort. There are various types of toenail fungus, each with distinct characteristics in symptoms and appearance. The most prevalent form is subungual onychomycosis, characterized by nail lifting, discoloration, and crumbling of the toenail. White superficial onychomycosis causes white, flaky patches on the nail surface, potentially progressing to rough and crumbly nails. Candida onychomycosis, caused by yeast, is more common in individuals with conditions like diabetes or compromised immune systems. This type of toenail fungus shows symptoms such as rough nails, surface breakdown, and soft tissue infection. An accurate diagnosis by a podiatrist is essential to determine the type of toenail fungus you may have incurred. With proper care and timely intervention, toenail fungus can be effectively managed. If you suspect you have a toenail fungus, it is suggested that you schedule an appointment with a podiatrist for an exam and treatment options appropriate to the cause.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Dr. Ronald K. Olm of Grand Traverse Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact one of our offices located in Traverse City and Kalkaska, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.





